



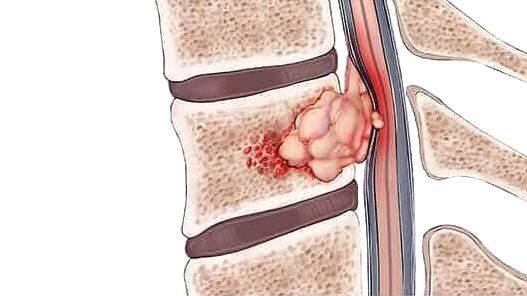
A spinal tumour is an abnormal growth of cells arising from any of the structures that constitute the spine. Our spine is a cylindrical structure made up of 33 vertebrae that are stacked one over the other, constituting the vertebral column, and serves to protect the spinal cord by proving a safe encasement. 31 pairs of spinal nerves emerge from the spinal cord and exit on either side of the vertebral column through apertures in the spinal column known as intervetebral foramina. The spinal cord and the roots of nerves that lie within the spinal canal have a sleeve around it formed by meninges. Spinal tumours can arise from any of these structures viz, spinal cord, spinal nerves, meninges, or the vertebrae. The growths that arise for the vertebral column are sometimes called vertebral tumours.

Spinal tumours can be classified into 4 types based on their geographical origin and location: those that originate within the spinal cord (intramedullary), from the nerve roots or the meninges covering the cord (intradural-extramedullary), between the covering dura and the bony column (extradural), and from the spinal column itself (vertebral).
Astrocytomas and ependymomas originate from the spinal cord, neurofibromas and schwannomas from nerves, meningiomas form the coverings, and metastases and chordomas from the bony column. Cancer of lungs and prostate are the commonest primary sites to spread to spine in males, and breast cancer the commonest in women.
Another way of categorizing spinal tumours is by their growth characteristics and propensity for cancer as either benign or malignant. Benign tumours are noncancerous and are slow to grow, whereas malignant tumours are cancerous and progress rapidly.
Tumours that begin first in the spine are called primary spinal tumours, and those that arise elsewhere in the body first and then spread to involve spine later on are called secondary or metastatic spinal tumours. Metastatic spinal tumours are much more common than primary spinal tumours, accounting for more than 95% of all spinal tumours. Though spinal cord and column are a continuation of brain and cranium, the tumours that arise in the brain outnumber that from spine by a factor of 4 to 1.
Spinal tumours can arise in any age group, but are more likely in patients who have cancers. Primary spinal cancers are rare, and occur mainly in people in their sixth and seventh decades of life, Though very rare, tumours of the spine can occur in children also, especially in their second decade.
What causes a spinal tumour to occur is still largely unknown. Causal relationship of chemicals to tumour formation have been hypothesized in some cases, whereas genetic basis in some tumours like neurofibromas is well established.
Pain is often the first symptom of a spinal tumour. One may experience pain at the mid-back or low back region as spinal tumours are most often located at these sites. At times pain can occur in a radial manner around the torso, or as shooting pain down your leg. Pain that doess not subside with rest, and which is more troublesome at night may serve to distinguish it from pain of muscular strains and pain from intervertebral disc compressions. Numbness or pins-n-needles sensation in the legs or arms is another symptom that is characteristic of neural involvement. A compression of the spinal cord or spinal nerves by a tumour can cause weakness in the limbs that may vary from mild affliction to total paralysis. Pressure on the lower part of spinal cord (known as cauda equina) can result in loss of bladder and bowel control leading to urinary or faecal incontinence, constipation etc. Muscle cramps, fatigue, loss of weight etc. may also be part of the symptom complex. Metastatic tumours may weaken the vertebrae and lead to their collapse precipitating acute severe pain sometimes associated with neurological deficits like inability to move a limb.
If you experience any of the above symptoms that are not going away in a months’ time, it is important to meet a healthcare practitioner, preferably one who is specializing in spine like a Neurosurgeon, or an Ortho-spinal surgeon, or a Neurologist. A clinical examination will elicit if there is tenderness (pain on deep pressing) in spine, or whether there are any neurological findings that are of concern. A diagnosis is established by sending the patient for imaging. An X-Ray examination of the part is a basic investigation to start with, alongside blood tests. Definitive diagnosis is arrived at from taking an MRI Scan of the concerned spinal region. MRI is a very safe investigation as it does not involve ionizing radiation. At times CT scan and PET scans may become necessary as supplementary investigations to complete the diagnostic picture.
Treatment of spinal tumours involves one of the 3 modalities: surgery, radiation therapy, and chemotherapy; either alone or in a combination. A multi-disciplinary team of surgeons, radiation oncologists, medical oncologists, neurophysiatrists and physiotherapists, and specialized nurses are involved in the care group.
In those patients in whom spinal tumours are asymptomatic, or only minimally symptomatic, observation by periodic check-ups is all that may be necessary. Tumours that have produced significant symptoms may require surgery. The goal of surgery is total removal by en bloc resection, which is possible in most benign tumours. In malignant tumours, this may not be feasible in all cases and maximal safe removal to whatever extent possible without entailing much neurological deficits, is undertaken.
‘Surgery’ evokes fear and consternation in the minds of nearly all people as to whether they will end up paralysed if subjected to it. This is a misplaced understanding and needs to be allayed. Techniques of various surgeries have evolved over the years and have incorporated layers of safety features that preclude major or inadvertent neurological hazards.
Spinal tumours are operated upon under high-definition and magnified vision provided by operating microscopes and endoscopes. Real-time assessment of neurological function is afforded through neuro-monitoring of electrical signals from neural tissues known as motor and sensory evoked potentials (MEPs and SEPs). Smaller benign tumours maybe amenable for removal through a key-hole with endoscopes. Spinal stabilization or reconstruction procedures by way of metallic implants are sometimes needed. An advanced technological aid known as Neuronavigation is made use for finding safe trajectories in spine for insertion and fixing of screws, rods, and cages in such cases.
Radiation therapy is given in malignant spinal tumors and delivered through specialized equipments. Intensity Modulated Radiation Therapy (IMRT) and Stereotactic Radiosurgery (SRS and SRT) by GammaKnife or CyberKnife are advanced techniques used for delivering radiation. Proton Beam Radiation is effective in certain malignant tumours.
Chemotherapy is adminstered for malignant tumours by Medical Oncologists. Treatment regimens would differ for each type of primary cancer that has metastasized to spine. Anti-cancer medications for a metastases or secondary spinal tumour that has originated from a primary in lungs or breast will vary, understandably.
Recovery and outcomes depend on the age of the patient and type of spinal tumour, and its site of origin. Benign tumours arising from nerve roots and meninges are often amenable to total surgical removal and cure. Primary tumours that arise from within spinal cord (like astrocytomas), or secondary tumours which are malignant are not always possible to be surgically removed. Some malignant cancers respond very well to radiation or chemotherapy, and their progression can be kept under check. A structured neurorehabilitative program is needed for those patients with weakness in limbs.
Patients need understanding and support from their family members. No efforts should be spared by all care-givers to keep them motivated, and in maintaining a positive frame of mind, which is very important in conquering the illness and the debility.
--------------------------------------------------------------------------------------------
Author:
Dr. THARUN KRISHNA
MBBS, D.Ortho, MS (General Surgery), M.Ch (Neurosurgery), IFAANS
Fellowships in: Spine Surgery (Germany),
Stereotactic and Functional Neurosurgery (Taiwan)
Senior Consultant Neurosurgeon and HoD
Apollo Adlux Hospital, Kochi, Kerala